
1.3M
Downloads
291
Episodes
A UK based Emergency Medicine podcast for anyone who works in emergency care. The St Emlyn ’s team are all passionate educators and clinicians who strive to bring you the best evidence based education. Our four pillars of learning are evidence-based medicine, clinical excellence, personal development and the philosophical overview of emergency care. We have a strong academic faculty and reputation for high quality education presented through multimedia platforms and articles. St Emlyn’s is a name given to a fictionalised emergency care system. This online clinical space is designed to allow clinical care to be discussed without compromising the safety or confidentiality of patients or clinicians.
A UK based Emergency Medicine podcast for anyone who works in emergency care. The St Emlyn ’s team are all passionate educators and clinicians who strive to bring you the best evidence based education. Our four pillars of learning are evidence-based medicine, clinical excellence, personal development and the philosophical overview of emergency care. We have a strong academic faculty and reputation for high quality education presented through multimedia platforms and articles. St Emlyn’s is a name given to a fictionalised emergency care system. This online clinical space is designed to allow clinical care to be discussed without compromising the safety or confidentiality of patients or clinicians.
Episodes

Monday Mar 20, 2023
Ep 212 - February 2023 Monthly Round Up
Monday Mar 20, 2023
Monday Mar 20, 2023
Our regular monthly round up and chat from the St Emlyn's blog. We talk about the use of artificial intelligence in research and the use of remifentanil instead of neuromuscular blockade in rapid sequence intubation. Plus more about the StEmlynsWILD conference and Simon's new role as Dean of RCEM and how you can get involved.

Monday Feb 27, 2023
Ep 211 - Semi structured interviews (CAN 9)
Monday Feb 27, 2023
Monday Feb 27, 2023
Long term listeners to the St Emlyn’s podcast may remember our series entitled ‘Critical Appraisal Nuggets’ (CANs). We are absolutely delighted to reinvigorate this project under the leadership of Professor Rick Body, with the episode on semi structured interviews.
In this easily digestible and succinct podcast Rick and Laura Howard go through the pros and cons of setting up semi structured interviews and how these can be used effectively in qualitative research.
In the latest episode, we cover a qualitative research technique: semi-structured interviews. Qualitative research might be out of your comfort zone: we’re generally more comfortable with quantitative measures – numbers and statistics. It’s something they have experience with, having previously published a paper exploring the impact of events that happen at work on the wellbeing of emergency physicians. This was a labour of love for Laura. Laura wrote a powerful blog about it here.
Semi-structured interviews are a great way to get the really rich data we need to understand something in greater depth. They allow us to ask ‘why?’ as well as just ‘what?’, ‘who?’ and ‘when?’. But reading qualitative research papers can be difficult when it takes us out of our comfort zone. In this CAN podcast, Laura and Rick take us through what semi-structured interviews are, why we might use them, how you design and conduct them, and they also have some pearls of wisdom about how to make transcribing them a lot less painful. By the end, we hope that you’ll feel confident with the basics of the technique. And if you want to practice your critical appraisal, why not put their study under the microscope?

Monday Jan 16, 2023
Ep 209 - November and December 2022 Round Up
Monday Jan 16, 2023
Monday Jan 16, 2023
A special double edition covering the blog posts from November and December and more. We discuss evidence based medicine with the DoseVF trial, and more from RECOVERY, discussion about 'what is downtime' and how we organise follow up for patients who don't live in our area and what happened at the amazing London Trauma Conference
We also announced some of the plans for StEmlynsWILD. Look out for booking details and more in the coming weeks.

Saturday Dec 10, 2022
Ep 208 - What is Wellbeing with Liz Crowe
Saturday Dec 10, 2022
Saturday Dec 10, 2022
Wellbeing is very complex, as it is an individual construct that is strongly aligned and interpreted through a lens of personal values, philosophy, culture, faith, and goals for life. Most importantly, wellbeing is dynamic rather than homeostatic and a subjective state determined by the individual.
Yet we use the term wellbeing to describe a wide variety of different things (often in terms of being the opposite of burnout which it most certainly isn't).
In this second episode of our series Liz Crowe discusses in detail what the literature says about wellbeing and how we may be able to use this going forward.
Please do like and subscribe. Thanks for listening.

Sunday Nov 27, 2022
Ep 207 - Burnout with Liz Crowe
Sunday Nov 27, 2022
Sunday Nov 27, 2022
Burnout is a term that seems to be used a lot these days, but what does it really mean? In this episode Dr Liz Crowe explains all, and will almost certainly change the way you view burnout.
Liz, who be well known to St Emyn's audiences, has just completed her PhD on "Understanding the risk and protective factors for burnout and wellbeing of staff working in the Paediatric Intensive Care Unit: PICU staff wellbeing" and has an unrivalled real world and evidence based experience of what these terms really mean.
In this first in a special series Liz goes into depth describing not only what burnout is, but how it can be measured (and the limitations of this) and most importantly how this is a system issue and not a diagnosis.
In the next episode we will discuss another commonly used term 'wellbeing'.
We think this series is incredibly important and hope you will help us share it far and wide. You can read the accompanying blogpost here.

Monday Nov 14, 2022
Ep 206 - October 2022 Round Up
Monday Nov 14, 2022
Monday Nov 14, 2022
In our new regular slot of the middle Monday of the month we're delighted to bring you the highlights from the St Emlyn's blog this month.,
Iain and Simon chat about batching in EDs, Ossilation in decision making and a whole lot more about trauma (chest drains, extrication, sex and TXA and rib fixation).
Please do like and subscribe and keep an eye out for our new sister website St Emlyn's Medical School and it's podcast series coming soon.

Saturday Oct 08, 2022
Ep 204 - August 2022 Round Up
Saturday Oct 08, 2022
Saturday Oct 08, 2022
This is our round up of all that happened on the St Emlyn's blog in August 2022 (yes - we know it's a bit late, but there's been a lot going on!).
Listen to Simon and Iain discuss the latest therapies in COVID, particularly Baricitinib, calcium in trauma and how we find balance in our work-life blend.
Please do like and subscribe to the podcast and tell your friends and colleagues. We've lots of exciting stuff coming your way over the next few months.

Sunday Aug 07, 2022
Ep 203 - June and July 2022 Round Up
Sunday Aug 07, 2022
Sunday Aug 07, 2022
Simon and Iain run through the latest highlights from the St Emlyn's blog and podcast, including the FORCE study, the EXIT study and more about Vitamin C in sepsis...
We hope you enjoy the podcast. Please do like and subscribe on your preferred podcast app and tell your friends and colleagues about us.

Thursday Jun 16, 2022
Ep 202 - May 2022 Round Up
Thursday Jun 16, 2022
Thursday Jun 16, 2022
Our monthly round up of all from the St Emlyn's blog. We discuss pathways into emergency care research, pad positioning in cardioversion of AF and possible gender differences in the presciption of TXA in trauma.
We also chat about travel in Lithuania, memories of defibrillating with hand held paddles and Simon's recent forst infection with COVID.
We mention a post on Lyme disease which you can read here (especially if you live near the New Forest...)

Thursday May 12, 2022
Ep 201 - March/April 2022 Round Up
Thursday May 12, 2022
Thursday May 12, 2022
After a brief hiatus we're back with more from the St Emlyn's Blog. We discuss a wide range of topics from crowding in Emergency Departments and the RePHILL trial to breastfeeding, genetic testing and diagnosing DVTs, as well as our highlights from the recent RCEM CPD Conference in Bournemouth. There really is something for everyone!

Thursday Jun 17, 2021
Ep 192 - May 2021 Round Up
Thursday Jun 17, 2021
Thursday Jun 17, 2021
It's been a busy month on the blog with plenty for Iain and Simon to talk about. The Manchester Arena bombing, new guidelines for Anaphylaxis management, Adult Congenital Heart Disease, Calcium in Major Haemorrhage and Spontaneous Coronary Artery Dissection all get a mention alongside the usual witterings of two middle aged emergency physicians.

Wednesday May 26, 2021
Ep 191 - Adult Congenital Heart Disease in the ED: Part 2
Wednesday May 26, 2021
Wednesday May 26, 2021
This is the second in a two part podcast series discussing Adult Congenital Heart Disease (ACHD) and how these patients may present to the Emergency Department (ED). Dr Sam Fitzsimmons, our guest on the podcast, is a Consultant in Adult Congenital Heart Disease at University Hospital Southampton. There is more information in this blog post.
In this episode we discuss Eisenmenger Syndrome, Transposition of the Great Arteries and Coarctation of the Aorta.

Thursday May 20, 2021
Ep 190 - Adult Congenital Heart Disease in the ED: Part 1
Thursday May 20, 2021
Thursday May 20, 2021
This is the first in a two part podcast series discussing Adult Congenital Heart Disease (ACHD) and how these patients may present to the Emergency Department (ED). Dr Sam Fitzsimmons, our guest on the podcast, is a Consultant in Adult Congenital Heart Disease at University Hospital Southampton. There is more information in this blog post.
Look out for Part 2, which will be released next week, where we discuss Eisenmenger Syndrome, Transposition of the Great Arteries and Coarctation of the Aorta.
Background
With advances in paediatric cardiac surgery, more and more patients with complex congenital heart disease are surviving to adulthood: in the 1950s you might expect a survival rate of about 10%, whereas now this is more like 85%. In fact, there are more patients in the adult congenital heart disease population than there are in the paediatric one (with 2.3 million adults vs 1.9 million children in Europe).
Many patients with Adult Congenital Heart Disease are young and able to live a relatively normal life. This means that they can travel and take part in just the same sort of activities as those without ACHD. They may well turn up in your Emergency Department one day, regardless of whether you are a tertiary centre or a district general hospital (DGH).
They are experts, and know their disease well, but this does not abstain you from a responsibility to know about them too! When these patients become unwell, they can go downhill very fast and you may not have the chance to discuss with them their exact lesion and its management.
The anatomy and physiology of these patients is abnormal, so they may present in atypical ways, and may not respond to usual medical interventions: in fact, some of our usual treatments may even be harmful.
However, starting with our usual 'ABC' approach is by far the best way to go, whilst gathering more information and contacting their specialist centre. Many patients will have their last clinic letter and ECG with them (which will also have the direct dial number of their specialist). And if they, or their relative, say there is something wrong you must believe them and do all you can to make sure they are fully investigated.
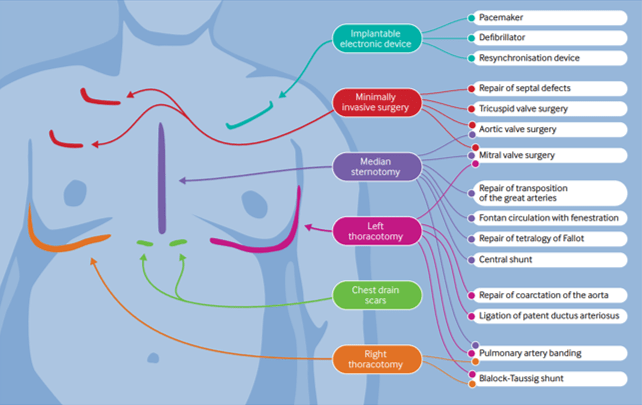
The presence of scars may give you some clues as to the patient's underlying condition and previous surgical repairs. (BMJ 2016; 354: i3905)
A General Approach
- Do your usual ABC assessment.
- Pay particular attention to the respiratory rate - this should be normal.
- Give oxygen if they look unwell.
- They should have a 'normal' blood pressure - any hypotension should be taken as abnormal and investigated.
The Fontan Circulation
This is not a condition in itself, but in fact the resulting circulation after a series of operations that could've been performed due to a number of different underlying conditions:
- Tricuspid Atresia
- Double Inlet Left Ventricle
- Atrio-ventricular Septal Defect – unbalanced
- Pulmonary Atresia
- Hypoplastic Left Heart Syndrome
In essence these patients are born with a single functioning ventricle, that has to be utilised to supply the systemic side of the circulation, whilst the Fontan acts as a passive means of returning blood to the pulmonary circulation.
It was first devised in the early 1970s by Dr Francis Fontan, so the majority of patients with this are in their mid thirties and younger.
Potential reasons for admission to the ED - Fontan circulation
1, Arrythmia
As the patient is entirely dependent on their systemic ventricle to work optimally, any disturbance of the delivery into it is very poorly tolerated. Thus, any arrhythmia is life threatening, even a mild atrial tachycardia.
These patients need to be returned to sinus rhythm as quickly as possible and the recommended method for this is DC cardioversion in expert hands.
Fontan patients have an incredibly fragile circulation and any change in their respiratory physiology can be life threatening, especially if it increases their pulmonary pressures (and thus prevents the passive flow within the Fontan circulation). These patients are not candidates for sedation in the ED and should have an experienced anaesthetist to manage them during the procedure.
Beware if the patient comes in and tells you they are fasted! This means they have been in this situation before and needed DC cardioversion.
2, Haemoptysis
Over time the patient develops venous hypertension within the Fontan connection. This causes the formation of collateral vessels, that may link into the bronchial arterial tree.
If the patient presents in shock treat them as you would any other patient with emergency blood transfusion.
Any haemoptysis, however small, may herald the beginning of a massive bleed. These patients need further investigation, probably a CT chest with contrast. These vessels may then be coiled by interventional radiology.
3, Cyanosis
If the patient has a non fenestrated Fontan they should have normal oxygen saturations. However, if there is a fenestration there will be shunting and therefore a reduction in oxygenation.
For patients this is trade of between being pink or blue, each of which have complications.
Dr Sam Fitzsimmons
Dr Sam Fitzsimmons is a Consultant Cardiologist in Adult Congenital Heart Disease (ACHD) at the University Hospital Southampton, UK. Sam also subspecialises in pulmonary hypertension and maternal cardiology. Working within a tertiary surgical ACHD centre, Sam delivers an ACHD on call service for emergency admissions, inpatient care, routine outpatient follow-up, intra-operative imaging and post-surgical care, as well as specialist clinics in Pulmonary Hypertension and Maternal Cardiology. Sam holds a Honorary Senior Clinical Lecturer post with the University of Southampton as she is passionate about teaching and in particular, she is enthusiastic about helping demystify congenital heart disease for many non-specialist to improve patient care. Sam is well published in peer review journals, cardiology textbooks and specialist guidelines.

Friday May 14, 2021
Ep 189 - April 2021 Round Up
Friday May 14, 2021
Friday May 14, 2021
A podcast with Iain and Simon summarising all the latest content from the St Emlyn's blog in April 2021. Topics discussed include Vaccine Induced Thrombocytopenic Thrombosis, how our own biases can effect our critical appraisal and whether we need to worry about grading the quality of FOAMed resources.
Thanks for listening. Please check out the blogs themselevs at www.stemlynsblog.org and consider subscribing and rating us on iTunes.
If you'd like to see some more from Peter Brindley you can watch one of his SMACC talks here.

Monday Mar 15, 2021
Ep 185 - February 2021 Round Up
Monday Mar 15, 2021
Monday Mar 15, 2021
Our regular podcast round up from February 2021. Iain and Simon highlight the key learning points from this month on the St Emlyn’s blog and podcast.
Topics discussed this month include tocilizumab in COVID19, TIA risk scores, new Emergency Care standards (targets) and TXA use in epistaxis. We also pay tribute to Dr Cliff Mann, former President of RCEM who sadly died this month.
Please remember to subscribe to the podcast on iTunes/Google Play and please do leave us some reviews and ratings there.

Sunday Jan 17, 2021
Ep 182 - COVID-19 vaccines update (January 2021)
Sunday Jan 17, 2021
Sunday Jan 17, 2021
A vaccine update with Rick Body, Simon Carley, Pam Vallely, Paul Klapper and Charlie Reynard. Bringing RCEM, St Emlyn's and the University of Manchester together for the latest thoughts and wisdom on the vaccines that might get us out of this pandemic.
Moderna vaccine phase 3 trial - https://www.nejm.org/doi/full/10.1056/nejmoa2022483
Oxford vaccine phase 2/3 - https://www.thelancet.com/pdfs/journals/lancet/PIIS0140-6736(20)32466-1.pdf
Pfizer vaccine trial - https://www.nejm.org/doi/full/10.1056/NEJMoa2034577
#vaccines #COVID19 #coronavirus

Thursday Dec 17, 2020
Ep 181 - Christmas 2020 Round Up
Thursday Dec 17, 2020
Thursday Dec 17, 2020
A special festive edition of our round up podcast featuring six weeks of blog posts and plenty more besides.
From all at St Emlyn's we hope you have a very happy festive season and we cannot wait to talk to you again in 2021.
Take care,
Simon and all the team

Friday Nov 06, 2020
Ep 179 - October 2020 Round Up
Friday Nov 06, 2020
Friday Nov 06, 2020
A bumper edition of the podcast where Iain and Simon discuss TXA (twice), antibiotics in appendicits, VTE, Blood products in trauma, use of ultrasound in cardiac arrest and plasma in traumatic brain injury. Oh, and COVID19 (but not for long)...
An evidence based cornucopia of aural pleasure.
Please like and subscribe (as all podcasters seem to say).
Take care,
Iain

Saturday Oct 24, 2020
Ep 178 - Surviving the Second Wave with Liz Crowe (October 2020)
Saturday Oct 24, 2020
Saturday Oct 24, 2020
In this special edition of the podcast, Liz Crowe discusses with Iain how we can find contentment, despite the relentless nature of COVID19 and the impending second wave. She gives practical, realistic advice that everyone can consider and encourages us all to be kind to ourselves in these strange and difficult times.
Wednesday Sep 23, 2020
Crackcast - Head Injury
Wednesday Sep 23, 2020
Wednesday Sep 23, 2020
This excellent epsiode of Crackcast covers all you need to know about head injury in the ED.

Thursday Sep 10, 2020
Ep 175 - August 2020 Round Up
Thursday Sep 10, 2020
Thursday Sep 10, 2020
Welcome to our audio round up of everything on the blog during August.
As the world continues to be in the grips of the Coronavirus pandemic there have been more papers looking at all aspects of this disease.
Simon reviewed the latest paper on Hydroxychloroquine and Charlie collated some of the top papers covering aspects from aerosol spread and use of CPAP to the effect on vulnerable groups and the effect on staff psychological health
It's not all COVID though. Sepsis is a condition we all want to be able to treat more effectively. Sadly there doesn't seem to be any encouraging news about the use of Vitamin C, Steroids and Thiamine in this latest RCT.
Many of the St Emlyn's group have special expertise in toxicology and Gareth wrote this incredibly informative post about the use of GBL. If you're not sure what "ChemSex" is then this post from a few years ago by Janos is worth a read.
The anonymously written "Look at what they make you give" post really struck a chord with readers, with an astonishing number of views. There are messages here for us all.
The numbers of Lesson Plans available continue to grow. We've had some great feedback following their use in induction. If tyou've not seen them yet, do have a look and let us know what you think.

Saturday Aug 01, 2020
Ep 174 - June and July 2020 Round Up
Saturday Aug 01, 2020
Saturday Aug 01, 2020
Our own version of Buy One Get One Free* this month, where you get a round up of two months of blog content.
Coronavirus continues to dominate the medical (and non-medical) headlines, and we discuss the two major results from the RECOVERY trial published recently, one positive and one not so (depending on who you talk to....). Simon also catches up with Roberto Cosentini, who you'll remember from the very powerful podcast at the beginning of the pandemic.
COVID isn't the only EBM circus in town though: we've reviewed HALT-IT and Simon has given a talk about the "Ten Top Trauma Papers" of the last year and Laura reviewed a paper looking at haloperidol for headaches.
We're having to think even harder about how we communicate in the ED, both for clinical care and to deliver education. Two ideas to help learning have been featured this month: The St Emlyn's Lesson Plans and "Background Learning".
Good luck to all those starting in Emergency Medicine, and a huge thank you to all those who are moving to other areas of medicine or other departments. It's been a curious few months...
Take care,
Iain
*It's actually Get One Free Get Another Free, but whose ever heard of that?

Thursday Jun 25, 2020
Ep 173 - The St Emlyn's Lesson Plans
Thursday Jun 25, 2020
Thursday Jun 25, 2020
We are delighted to introduce you to the "St Emlyn's Lesson Plans", which we hope will help structure some of your education sessions over coming months (and years).
Each lesson plan starts with a descrete learning outcome, to set the scene, as well as details of the RCEM curriculum item(s) that will be covered.
The first tasks are aimed at aquiring some background knowledge and can either be done as part of the session, or beforehand. These utilise the vast "FOAMed" resources (including, but not exclusively, those of St Emlyn's).
Our experience is that time constraints often mean that "background reading" isn't achieved before the session, so would encourage allowing time within it to complete these. They are designed to take about 30 minutes and occupy the first half of the session.
Everything you need for each lesson is included in the plan. We would recommend that each learner has an internet enabled device available (with headphones) to read and listen to the background material at their own pace.
The second half of the session should be facilitated by an expert. This can happen in person, but also online, via any of the interfaces that are now so familiar.
In many plans we have given some case examples, but it would be even better if learners can bring cases of their own for discussion. This element is very much within the control of the facilitator (who should been fully cogniscent of the contents of the knowledge section).
The session finishes off with a summary, this should emphasise again the most important learning points. To really embed the knowledge and skills the particiapants should be encouraged to reflect on what they have learned, and to even talk to thse who were unable to attend about what they missed.
For learners this also gives an opportunity to easily link teaching sessions to their portfolio.
You may want to record the "face-to-face" elements, so that those who were not present are able to access them when they can (and those that did can rewatch to refresh their learning).
Although these plans are designed for delivery in a single centre, there is absolutely no reason why regional (or even national) teaching could take place in this way. The recent COVID19 Journal Clubs have demonstrated beautifully how a group of learners can engage with an online panel.
We would be very happy to receive lessons plans to add to the collection. This is very much a collaborative effort.
Please let us know what you think of these lesson plans and if you are using them in your Department. We'd love to hear your ideas about how we can take medical education forward.

Friday Jun 19, 2020
Ep 172 - Dexamethasone and COVID - Show us the Data! (June 2020)
Friday Jun 19, 2020
Friday Jun 19, 2020
St Emlyn's three professors, Carley, Body and Horner* critically appraise the Press Release regarding Dexamethasone in the treatment of COVID-19.
What does this mean for the future of Evidence Based Medicine? Can we really start using a medication when the trial hasn't been peer reviewed and the full dataset not released?
The blog post by Josh Farkas, that is mentioned in the podcast, is here.
*Professor Simon Carley, Professor of Emergency Medicine at Manchester Metropolitan University and a Consultant in Adult and Paediatric Emergency Medicine at Manchester Foundation Trust, Professor Rick Body Professor of Emergency Medicine in Manchester and Honorary Consultant in Emergency Medicine at Manchester Foundation Trust. Professor Dan Horner, Professor of Emergency Medicine of the Royal College of Emergency Medicine and Consultant in Emergency Medicine and Intensive Care at Salford Royal NHS Foundation Trust.

Thursday Jun 04, 2020
Ep 170 - COVID-19 Journal Club #7 (June 2020)
Thursday Jun 04, 2020
Thursday Jun 04, 2020
Welcome to our seventh webinar and journal club reviewing recent research and featuring COVID-19 updates, hosted by the University of Manchester, Manchester Royal Infirmary and Royal College of Emergency Medicine in collaboration with St Emlyn's.
The live event took place on Tuesday 26th May.
Today's panel will be hosted by Rick Body The panel includes Prof Paul Klapper (Professor of Clinical Virology), Dr Charlie Reynard (NIHR Clinical Research Fellow), Dr Anisa Jafar, Prof Pam Vallely (Professor of Medical Virology), Ellie Hothershall (Consultant in Public Health), Prof Simon Carley and special guest Kelly Ann Janssens (Emergency Physician in Ireland) to discuss five papers about COVID-19 infection.
This will be the last weekly journal club, but we will be back with more EBM goodness very soon. Do let us know what you like to be included at stemlyns@gmail.com
References
-
Beigel JH, Tomashek KM, Dodd LE, et al. Remdesivir for the Treatment of Covid-19 — Preliminary Report. N Engl J Med. Published online May 22, 2020. doi:10.1056/nejmoa2007764
-
Mehra MR, Desai SS, Ruschitzka F, Patel AN. Hydroxychloroquine or chloroquine with or without a macrolide for treatment of COVID-19: a multinational registry analysis. The Lancet. Published online May 2020. doi:10.1016/s0140-6736(20)31180-6
-
Gray N, Calleja D, Wimbush A, et al. “No test is better than a bad test”: Impact of diagnostic uncertainty in mass testing on the spread of Covid-19. Published online April 22, 2020. doi:10.1101/2020.04.16.20067884
-
Peyrony O, Marbeuf-Gueye C, Truong V, et al. Accuracy of Emergency Department clinical findings for diagnostic of coronavirus disease-2019. Annals of Emergency Medicine. Published online May 2020. doi:10.1016/j.annemergmed.2020.05.022
-
Ludvigsson JF. Children are unlikely to be the main drivers of the COVID‐19 pandemic – a systematic review. Acta Paediatr. Published online May 19, 2020. doi:10.1111/apa.15371

Friday May 22, 2020
Ep 169 - COVID-19 Journal Club #6 (May 2020)
Friday May 22, 2020
Friday May 22, 2020
Welcome to our sixth COVID-19 Journal Club Podcast.
The panel was hosted by Rick Body and included Prof Paul Klapper (Professor of Clinical Virology), Dr Charlie Reynard (NIHR Clinical Research Fellow), Dr Anisa Jafar, Prof Pam Vallely (Professor of Medical Virology), Prof Simon Carley and special guest Liz Crowe (Advanced Clinician Social Worker and PhD candidate in health staff wellbeing in Brisbane) to discuss four papers about COVID-19 infection. We were especially pleased to welcome Liz this week, which enabled us to focus on the important topics of grief, loss and communication during the COVID-19 pandemic.
References

Friday May 15, 2020
Ep 168 - COVID-19 Journal Club #5 (May 2020)
Friday May 15, 2020
Friday May 15, 2020
Welcome to our fifth webinar and journal club reviewing recent research and featuring COVID-19 updates, hosted by the University of Manchester, Manchester Royal Infirmary and Royal College of Emergency Medicine in collaboration with St Emlyn’s.
The live event took place on Tuesday 12th May at 11.00am BST (10.00am GMT).
The COVID-19 Journal Club Panel
Today’s panel was hosted by Rick Body The panel includes Prof Paul Klapper (Professor of Clinical Virology), Dr Charlie Reynard (NIHR Clinical Research Fellow), Prof Dan Horner, Dr Anisa Jafar, Prof Pam Vallely (Professor of Medical Virology), Prof Simon Carley and special guest Lauren Westafer (Attending in Emergency Medicine and Co-Creator of the Foamcast blog and podcast) and Ellie Hothershall (head of undergraduate medicine at the University of Dundee and an expert in Public Health) to discuss six papers about COVID-19 infection.

Wednesday May 13, 2020
Ep 167 - Troponin Update and LoDED Study Review with Rick Body
Wednesday May 13, 2020
Wednesday May 13, 2020
Over the last few years many of us in the UK have started to incorporate high-sensitivity troponin into the assessment of patients presenting with chest pain.
We have seen these samples taken at ever shorter intervals, aiming to discharge low risk patients safely, sooner from the Emergency Department (ED). This has been driven in part by the "Four Hour Emergency Access Target" as well as increased crowding in overwhelmed EDs.
In this podcast, internationally renowned researcher Prof Rick Body discusses the latest in troponin research and the recent LoDED study.
The Shownotes
The various organisations mentioned by Rick can be found here:
The Innovation Agency Webinar Series
The NHS Accelerated Access Collaborative
The CQUIN that will be implemented later this year (page 15 for the Troponin section)
The Draft NICE recommendations

Thursday May 07, 2020
Ep 166 - COVID-19 Journal Club #4 (May 2020)
Thursday May 07, 2020
Thursday May 07, 2020
Welcome to our fourth webinar and journal club reviewing recent research and featuring COVID-19 updates, hosted by the University of Manchester, Manchester Royal Infirmary and Royal College of Emergency Medicine in collaboration with St Emlyn's.
The live event tool place on Tuesday 5th May at 11.30am BST (10.30am GMT).
The panel was again be hosted by Rick Body The panel includes Prof Paul Klapper (Professor of Clinical Virology), Dr Charlie Reynard (NIHR Clinical Research Fellow), Dr Anisa Jafar (Academic Clinical Lecturer), Prof Pam Vallely (Professor of Medical Virology), Prof Simon Carley and special guest Justin Morgenstern to discuss six papers about COVID-19 infection.
There will be another COVID 19 Journal Club next week (Tuesday 12th May at 11am).
References
Podcast edited from a live webinar by Izzy Carley

Sunday May 03, 2020
Ep 165 - April 2020 Round Up
Sunday May 03, 2020
Sunday May 03, 2020
It's been another busy month at St Emlyn's, with the publication of 15 blog posts and five podcasts, but there does seem to be an awful lot to talk about!
Of course there have been multiple posts and podcasts about COVID-19, and you can fiind all of these on our special St Emlyn's page. Highlights have included the three RCEM/St Emlyn's Webinars which we are delighted to host in podcast form.
It's not just been coronavirus though, we have also dipped out toes into exercise and nutrition, graphic design and horticulture!
Parts of the site have also undergone a bit of a redesign with the curriculum pages now easier to navigate to find that post to fioll an e-portfolio hole.
We hope you're finding all of our output useful. Please do subscribe to the website (in the top right hand corner) and rate our podcast on iTunes.
They'll be much more to come in May I am sure.
Take care
Iain
Podcast edited by Izzy Carley

Thursday Apr 30, 2020
Ep 164 - COVID-19 Journal Club #3
Thursday Apr 30, 2020
Thursday Apr 30, 2020
Welcome to our third webinar and journal club reviewing recent research and featuring COVID-19 updates, hosted by the University of Manchester, Manchester Royal Infirmary and Royal College of Emergency Medicine in collaboration with St Emlyn’s.
The live event took place on Tuesday 28th April at 11am BST (10am GMT).
The panel was hosted by Rick Body The panel includes Prof Paul Klapper (Professor of Clinical Virology), Dr Charlie Reynard (NIHR Clinical Research Fellow), Dr Dan Horner (RCEM Professor), Prof Pam Vallely (Professor of Medical Virology), Salim Rezaie (Emergency Physician and Founder of REBEL EM) and Prof Simon Carley (you know him…) to discuss five papers about COVID-19 infection. There will be another COVID 19 Journal Club next week (Tuesday 5th May at 11am).
Edited by Izzy Carley and Iain Beardsell
References
-
Helms J. High risk of thrombosis in patients in severe SARS-CoV-2 infection: a multicenter prospective cohort study. Intensive Care Medicine. April 2020:1-21. https://www.esicm.org/wp-content/uploads/2020/04/863_author_proof.pdf.
-
Caputo ND, Strayer RJ, Levitan R. Early Self‐Proning in Awake, Non‐intubated Patients in the Emergency Department: A Single ED’s Experience during the COVID‐19 Pandemic. Acad Emerg Med. April 2020. doi:10.1111/acem.13994
-
Garcia FP, Perez Tanoira R, Romanyk Cabrera JP, Arroyo Serrano T, Gomez Herruz P, Cuadros Gonzalez J. Rapid diagnosis of SARS-CoV-2 infection by detecting IgG and IgM antibodies with an immunochromatographic device: a prospective single-center study. April 2020. doi:10.1101/2020.04.11.20062158
-
Richardson S, Hirsch JS, Narasimhan M, et al. Presenting Characteristics, Comorbidities, and Outcomes Among 5700 Patients Hospitalized With COVID-19 in the New York City Area. JAMA. April 2020. doi:10.1001/jama.2020.6775
-
Metzler B, Siostrzonek P, Binder R, Bauer A, Reinstadler S. Decline of acute coronary syndrome admissions in Austria since the outbreak of COVID-19: the pandemic response causes cardiac collateral damage. Eur Heart J. April 2020. doi:10.1093/eurheartj/ehaa314

Saturday Apr 25, 2020
Ep 163 - COVID-19 Journal Club #2
Saturday Apr 25, 2020
Saturday Apr 25, 2020
Welcome to our second webinar on recent research about COVID-19, hosted by the University of Manchester, Manchester Royal Infirmary and Royal College of Emergency Medicine in collaboration with St Emlyn’s.
The panel was hosted by Rick Body. The panel includes Prof Paul Klapper (Professor of Clinical Virology), Dr Charlie Reynard (NIHR Clinical Research Fellow), Prof Pam Vallely (Professor of Medical Virology), Dr Anisa Jafar (Academic Clinical Lecturer), Dr Casey Parker and Prof Simon Carley (you know him…) to discuss six papers about COVID-19 infection.
The live event took place on Tuesday 21st April 2020
References:
Paper 1 (00:00) Tang W, Cao Z, Han M, et al. Hydroxychloroquine in patients with COVID-19: an open-label, randomized, controlled trial. April 2020. doi:10.1101/2020.04.10.20060558

Wednesday Apr 15, 2020
Ep 161 - COVID-19 Journal Club #1
Wednesday Apr 15, 2020
Wednesday Apr 15, 2020
Professor Rick Body is joined by Prof Paul Klapper (Professor of Clinical Virology), Dr Charlie Reynolds (NIHR Clinical Research Fellow), Prof Pam Vallely (Professor of Medical Virology), Dr Anisa Jafar (Academic Clinical Lecturer) and Prof Simon Carley (you know him...) to discuss six papers about COVID-19 infection.
03:10 - Paper 1 – Guan et al. Clinical characteristics of Coronavirus disease 2019 in China. NEJM Feb 28 2020
https://www.nejm.org/doi/full/10.1056/NEJMoa2002032
16:54 Paper 2 – Zou et al. Single Cell RNA-SEQ Data Analysis on the receptor ACE2 expression reveals the potential risk of different human organs vulnerable to 2019-NCOV infection. Frontiers of Medicine. Mar 12 2020.
https://link.springer.com/content/pdf/10.1007/s11684-020-0754-0.pdf
21:43 Paper 3 – Gautret et al. Hydroxychloroquine and azithromycin treatment of COVID-19: Results of an open-label non-randomised clinical trial. International Journal of Antimicrobial Agents. 20 Mar 2020
https://www.sciencedirect.com/science/article/pii/S0924857920300996?via%3Dihub
25:25 Paper 4 – Cao et al. A trial of Lopinavir-Ritonavir in adults hospitalized with severe COVID-19. NEJM Mar 18 2020
https://www.nejm.org/doi/pdf/10.1056/NEJMoa2001282
29:35 Paper 5 – Cui et al. Prevalence of venous thromboembolism in patients with severe Coronavirus pneumonia. Journal of Thrombosis and Haemostasis. Apr 9 2020 doi:10.1111/jth.14830
https://onlinelibrary.wiley.com/doi/epdf/10.1111/jth.14830
34:14 Paper 6 – Lynarts et al. Prediction models for diagnosis and prognosis of COVID-19 infection: systematic review and critical appraisal. BMJ. Apr 7 2020 BMJ 2020;369:m1328

Sunday Apr 05, 2020
Ep 160 - March 2020 Round Up
Sunday Apr 05, 2020
Sunday Apr 05, 2020
Iain and Simon discuss Covid19 and more in this review of the best of the blog from March 2020.

Thursday Apr 02, 2020
Thursday Apr 02, 2020
Simon interviews Dr John Rogers and Dr Nathan Lewis on respiratory infection prevention.
John a Sports and Exercise Medicine Consultant in Manchester. He is also Chief Medical Officer for British Triathlon and Visiting Professor in Sport & Exercise Medicine at Manchester Metropolitan University.
Nathan is lead performance nutrition scientist at the English Institute of Sport and at ORRECO.
These two academics take us through how sports science might be able to support our wellbeing during the Covid19 pandemic.
References
- Recommendations to maintain immune health in athletes https://www.tandfonline.com/loi/tejs20
- Probiotics https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD006895.pub3/epdf/full
- Vitamin D and Respiratory Tract Infections: A Systematic Review and Meta-Analysis of Randomized Controlled Trials https://pubmed.ncbi.nlm.nih.gov/23840373/
- Vitamin C for prevention and treatment of pneumonia https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD013134/full
- Vitamin C and common cold https://www.cochrane.org/CD000980/ARI_vitamin-c-for-preventing-and-treating-the-common-cold
- Effect of Flavonoids on Upper Respiratory Tract Infections and Immune Function: A Systematic Review and Meta-Analysis https://pubmed.ncbi.nlm.nih.gov/27184276/
- Vitamin C and Infections https://pubmed.ncbi.nlm.nih.gov/28353648/
- Zinc lozenges and the common cold: a meta-analysis comparing zinc acetate and zinc gluconate, and the role of zinc dosage https://pubmed.ncbi.nlm.nih.gov/28515951/

Sunday Mar 29, 2020
Ep 158 - Understanding Fear and Anxiety around COVID19 with Liz Crowe
Sunday Mar 29, 2020
Sunday Mar 29, 2020
The world is consumed by the Coronavirus pandemic, but how do we look after ourselves? Liz and Iain discuss some strategies to stay well over the coming weeks and months. Recorded on 25th March 2020.

Tuesday Mar 24, 2020
Ep 157 - ICU for the non-intensivist with Sarah Thorton
Tuesday Mar 24, 2020
Tuesday Mar 24, 2020
Simon chats to Sarah Thornton, consultant anaesthetist, intensivist and head of the NW school of anaesthesia on preparing to work in a critical care unit during the Covid-19 pandemic.

Friday Mar 20, 2020
Ep 156 - February 2020 Round Up
Friday Mar 20, 2020
Friday Mar 20, 2020
Iain and Simon chat about the current Corona pandemic and the blog in Feb 2020.
Iain remains positive, but Simon thinks the glass is half full. Time will tell who is right (though in truth there is a lot of common ground).
S

Saturday Mar 14, 2020
Ep 155 - Covid-19 Podcast from Italy with Roberto Cosentini March 2020
Saturday Mar 14, 2020
Saturday Mar 14, 2020
Dr Roberto Cosentini is an old friend of St Emlyn's who works in Bergamo, in Northern Italy. He is right at the heart of the recent Covid19 outbreak. He kindly found an hour to record a podcast with us on his experiences.
There are so many essential lessons in this podcast. Please share with clinical and non-clinical colleagues, as we need to plan NOW. Roberto is quite clear that if we don't train and get plans into place before the wave of cases hit us then both ourselves and our patients will suffer.
In the interest of speed I'm not going to summarise the whole podcast. You have to listen to it all yourself to see what's relevant to you. These are some of my take away messages.
- Divide your department into resp patients and non-resp patients
- Wear PPE and know how to use it
- You will need clinicians who do not usually work in ED. Train and orientate them now (before you need them).
- Most patients are hypoxic and this responds to O2 and CPAP. You're going to need a lot of CPAP and how that happens could be tricky. They found hoods the best (Ed - but how many of those do we have?).
- Although hypoxic, patients have good lung compliance.
- They regularly saw diurnal variation with many patients presenting in the early afternoon.
- It's emotionally exhausting. Prepare yourself and your team psychologically and support them during the pandemic. Roberto's department has an embedded psychologist.
- Health care worker infections were quite low (because they wore PPE for all resp cases).
- Flow through the department and onto wards is absolutely vital.
- Flow out the the main hospitals to other units that can rehabilitate is vital.
- Decisions for ICU level care were similar to normal (in his hospital)
We rarely declare one of our podcasts a 'must listen' but this is an exception. Please listen and share widely. Please think hard about the issues Roberto raises and PLEASE ACT NOW.
vb
S
How you can support St Emlyn's
- Join us for #stemlynsLIVE conference May 12th 2020
- Subscribe to the blog (look top right for the link)
- Subscribe to our PODCAST on iTunes
- Follow us on twitter @stemlyns
- PLEASE Like us on Facebook
- Find out more about the St.Emlyn’s team
- Find out more about the MMU MSc in Emergency Medicine here.
- Download one of our FREE e-books here


Wednesday Feb 12, 2020
Ep 154 - January 2020 Round Up
Wednesday Feb 12, 2020
Wednesday Feb 12, 2020
Iain is back on the podcast with Simon to talk through the best of the blog from January 2020.

Monday Dec 23, 2019
Ep 152 - November podcast round up on St Emlyn's
Monday Dec 23, 2019
Monday Dec 23, 2019
The latest from the St Emlyn's blog

Saturday Dec 07, 2019
Ep 151 - October 2019 Round Up
Saturday Dec 07, 2019
Saturday Dec 07, 2019
St Emlyn's October 2019 Round-Up: Key Insights from Conferences and Research
October 2019 was a bustling month for the St Emlyn's team, filled with important conferences, groundbreaking research, and engaging discussions in emergency medicine. This round-up covers the highlights, from tactical trauma insights to controversial trial results, providing a comprehensive overview of the month’s most significant developments.
Tactical Trauma Conference in Sundsvall, Sweden
The month started with the Tactical Trauma Conference in Sundsvall, Sweden, where Pete Hume, a colleague from Virchester, presented on the response to the Manchester Arena bombing. This tragic event, involving many pediatric casualties, posed significant challenges in managing a high volume of injured children. Pete’s presentation highlighted the crucial lessons learned during the response, emphasizing the importance of preparedness and efficient resource management.
A standout talk at the conference was given by Geoff Yost, who discussed the 2017 Las Vegas shooting. A key takeaway from his presentation was the importance of utilizing bystanders during mass casualty incidents. Bystanders are often the first to respond, and their actions can significantly influence outcomes. This was exemplified by the recent London Bridge attack, where members of the public intervened using improvised weapons like a narwhal tusk.
Pete also provided insights into leadership in crisis situations, a topic covered by Kate Pryor at the conference. Overall, the Tactical Trauma Conference underscored the need for collaboration with bystanders and the importance of effective leadership during emergencies.
R.CEM Annual Scientific Conference in Gateshead
The R.CEM Annual Scientific Conference, held in Gateshead at the end of October, brought together emergency clinicians, nurses, paramedics, and researchers to discuss the latest developments in emergency medicine. Chris Gray, a member of the St Emlyn's team, attended and shared his experiences through a series of blog posts.
One of the most anticipated studies discussed at the conference was the NOPE PAX study on the use of tranexamic acid for treating nosebleeds. Although the results are not yet publicly available, the study is expected to provide valuable insights into this increasingly popular treatment. Another key study was the CAP-IT study, which focuses on the use of antibiotics in pediatric pneumonia—a topic of ongoing debate in the context of antibiotic stewardship.
The conference also featured discussions on the CRASH-3 trial, particularly concerning the use of tranexamic acid in traumatic brain injury. Ian Roberts delivered a compelling presentation on the mechanisms of tranexamic acid and the significant differences in its use across various regions, including the UK, the US, and Australasia.
The TERN Network and the TIRED Study
A major highlight of the R.CEM conference was the presentation of the TIRED study, the first major project from the Trainees Emergency Research Network (TERN). Led by Dan Horner, the study surveyed the levels of fatigue among emergency physicians across the UK, using the Need for Recovery Score to assess recovery time after shifts.
The study revealed concerning results, with emergency clinicians scoring an average of 73 on the Need for Recovery Score, significantly higher than the previous highest score of 55 recorded for Iranian miners. This suggests that emergency clinicians are under immense pressure, leading to high levels of fatigue.
Interestingly, older clinicians had lower scores, indicating either greater resilience or better workload management. However, the study raises the controversial question of whether the job’s demands are causing some clinicians to leave the profession early.
The TERN network is continuing to explore critical questions in emergency medicine, with upcoming studies on subarachnoid hemorrhage and the necessity of lumbar punctures.
European Resuscitation Council Meeting in Slovenia
The European Resuscitation Council meeting in Slovenia was another key event in October. The chain of survival—early recognition, CPR, defibrillation, and post-resuscitation care—was a major focus of the conference. While much attention is often given to post-resuscitation care, the most significant impact on survival comes from the early stages of the chain.
The GoodSAM app, which allows trained responders to be notified of nearby emergencies, plays a crucial role in this early response. The app has already made a significant difference in several cases, including cardiac arrests.
Another important discussion at the conference was the use of hypothermia in post-cardiac arrest care. Following the TTM1 trial, which suggested that hypothermia might not be as beneficial as once thought, some clinicians have stopped temperature management altogether. However, evidence presented at the ERC meeting indicates that this may have led to an increase in post-arrest mortality. The ongoing TTM2 trial aims to provide more clarity on the role of hypothermia in post-cardiac arrest care.
Thromboprophylaxis in Lower Limb Immobilization
Dan Horner’s study on thromboprophylaxis in lower limb immobilization is another significant piece of research published this month. The study, a systematic review, highlighted that the incidence of significant deep vein thrombosis (DVT) in patients with lower limb immobilization is around 2%, and anticoagulation almost certainly reduces this risk.
However, the study also pointed out that there is no clear consensus on which risk stratification tool is best for identifying patients at risk of DVT. The GemNet guidelines from R.CEM are a solid option, but more research is needed in this area. The study also discussed the choice of anticoagulant, noting that while low-molecular-weight heparin is the most commonly used, the use of DOACs, such as rivaroxaban, is on the rise.
As an emergency physician, the balance between preventing life-threatening complications like pulmonary embolism and avoiding significant bleeding events remains a critical consideration in patient care.
Top 10 Papers from 2018-2019
The R.CEM Annual Scientific Conference also featured a presentation on the top 10 papers from the past year, covering a wide range of topics in emergency medicine.
One key study explored whether early or delayed cardioversion should be performed in recent-onset atrial fibrillation, with the conclusion leaning towards not immediately intervening. Another study examined whether ventilation should continue during RSI (rapid sequence induction), with evidence suggesting that it should.
The debate over cricoid pressure during RSI continues, with recent evidence indicating that it may not be necessary and could even be harmful in some cases. Magnesium in atrial fibrillation was also discussed, with the evidence supporting its use, particularly when combined with other treatments.
The presentation also covered the use of vasopressors in hemorrhagic shock, with early evidence suggesting they might be beneficial, though more research is needed. Finally, the discussion touched on diagnosing pulmonary embolism in pregnancy using the YEARS score, a promising but still developing area of research.
The CRASH-3 Trial: A Controversial Conclusion
The CRASH-3 trial, focusing on the use of tranexamic acid in traumatic brain injury, has generated significant debate in the emergency medicine community. While the trial’s findings have already started to influence practice in the UK, the way the results were interpreted and publicized has been controversial.
The debate centres around two main camps: one that argues the trial didn’t conclusively prove that tranexamic acid reduces mortality in traumatic brain injury and another that believes the evidence strongly suggests a benefit in certain subgroups. While not the final word on the subject, the CRASH-3 trial provides enough evidence to justify the use of tranexamic acid in specific scenarios.
Looking Ahead
As October ends and November begins, there’s much to look forward to. The Asian Conference of Emergency Medicine in India promises to be an exciting event, and the Resuscitology Conference in December is already sold out, with plans to run it again in 2020.
Emergency medicine is more intense than ever, with record numbers of patients and some of the toughest days experienced in the field. Despite these challenges, the St Emlyn's team continues to provide exceptional care and remain at the forefront of emergency medicine research and practice.
Thank you for following along with this month’s round-up. Stay tuned for more updates from St Emlyn's as we continue to explore, learn, and share the latest in emergency medicine.

Saturday Nov 02, 2019
Ep 149 - September 2019 Round Up
Saturday Nov 02, 2019
Saturday Nov 02, 2019
A Month in Review: Key Takeaways from St Emlyn's September 2019 Content
Welcome to a detailed overview of the latest content from St Emlyn's, focusing on the valuable insights and educational resources we shared throughout September 2019. This month’s offerings span a wide range of topics, from the evolving concept of the "resuscitationist" to the increasing challenges posed by decompensated liver disease, and the ongoing development of emergency medicine education. Here’s a look at the most important takeaways.
The Resuscitationist: More Than Just a Title
The term "resuscitationist" has become a buzzword within the emergency medicine (EM) and critical care communities, especially following its emergence from the SMACC (Social Media and Critical Care) conferences. Dan Horner delved into this concept in a recent presentation, sparking a broader discussion about what it truly means to identify as a resuscitationist.
At its core, being a resuscitationist isn’t just about having an interest in the resuscitation room. It requires a blend of sharp clinical skills, deep knowledge of resuscitation science, and the ability to apply evidence-based practices effectively. But beyond technical expertise, leadership and teamwork are crucial. A resuscitationist must excel in managing high-stakes, chaotic situations where decisions are made with limited information and under intense time pressure.
Moreover, Dan highlights the importance of humility and collaboration. The best resuscitationists are those who recognize their own limitations and are skilled at drawing on the strengths of others, whether from different specialties or professions. This collaborative approach not only enhances patient care but also builds stronger, more effective resuscitation teams.
Decompensated Liver Disease: A Growing Concern in the ED
Liver disease is on the rise, particularly due to lifestyle factors like alcohol consumption and obesity. Gareth Roberts tackled this pressing issue in his blog post on decompensated liver disease, which is becoming increasingly common in emergency departments (EDs) across the UK and beyond.
Gareth outlines a comprehensive care bundle designed to manage patients with decompensated liver disease effectively. This bundle includes seven key points:
-
Thorough Investigation: Quick and accurate investigations are essential, particularly for detecting complications like spontaneous bacterial peritonitis (SBP), which can be life-threatening.
-
Infection Management: Aggressive treatment of infections is critical, with a focus on using appropriate antibiotics and monitoring for SBP.
-
Acute Kidney Injury (AKI) and Hyponatremia: These complications are common in liver disease patients and must be managed carefully. Gareth discusses the potential benefits of human albumin in these cases.
-
GI Bleeding: Gastrointestinal bleeding, especially from varices, poses a significant risk. Gareth directs readers to additional resources on St Emlyn’s, including a presentation by Chris Gray on managing GI bleeding.
-
Hepatic Encephalopathy: This condition can severely alter a patient’s mental status and requires careful management. With the increasing prevalence of liver disease, understanding and managing hepatic encephalopathy is more important than ever.
Gareth’s post is a must-read for anyone dealing with liver disease in the ED, providing both practical advice and links to further resources.
Expanding Education: The MSc in Emergency Medicine
Education is a cornerstone of St Emlyn’s, and we’re excited to announce the expansion of the MSc in Emergency Medicine at Manchester Metropolitan University. This program has been running successfully for several years and is now broadening its scope to include paramedics, making it a truly multi-professional and multi-disciplinary course.
The MSc program offers a variety of modules tailored to the specific needs of different healthcare professionals. Whether you’re looking to deepen your clinical knowledge, enhance your leadership skills, or explore new areas of emergency medicine, this program has something to offer. For more details, visit our website or reach out directly.
Supporting St Emlyn’s: Keep Our Content Free and Accessible
St Emlyn’s remains committed to providing free and open-access content to the global emergency medicine community. However, maintaining and expanding our offerings requires resources. If you find value in what we provide, please consider supporting us financially. Even a small contribution can help us continue to deliver high-quality content to healthcare professionals worldwide.
Introducing Coda: The Next Evolution After SMACC
Coda is the latest evolution in the SMACC legacy, aiming to broaden the scope of its predecessor by incorporating a wider range of specialties, including oncology, public health, and surgery. As a member of the Coda executive team, I can attest to the ambitious goals of this new conference series.
Coda retains the clinical excellence that SMACC was known for, but with an added emphasis on advocacy. Each year, Coda will tackle a significant global health issue, with the inaugural theme focusing on climate change and its impact on medical practice.
It’s important to note that while climate change is a key focus, it won’t dominate the entire conference. Only about 25% of the program will be dedicated to this theme, with the remaining 75% featuring the high-quality clinical content you’ve come to expect from SMACC. The first Coda conference is set to take place in Melbourne in 2020, and we encourage you to participate, whether in person or remotely.
The Zero Point Survey: A Game-Changer in Resuscitation
The Zero Point Survey, a concept championed by Cliff Reid, is gaining widespread recognition for its transformative impact on resuscitation practices. The idea shifts the focus of the primary survey in resuscitation from when you first encounter the patient to what you do before you even meet them.
This approach emphasizes the importance of preparation—both mental and environmental. By optimizing everything you can control before the patient arrives, you set the stage for delivering high-quality care when it matters most.
Feedback from the EM community has been overwhelmingly positive, with many clinicians reporting that the Zero Point Survey has changed how they manage the resuscitation room. It’s not just a theoretical concept; it’s a practical tool that’s making a real difference in patient outcomes.
If you’re not yet familiar with the Zero Point Survey, I strongly encourage you to explore the resources available on the St Emlyn’s website, including an excellent video by Cliff Reid that outlines the key elements of this approach.
Looking Ahead: What’s Next for St Emlyn’s?
As we wrap up our review of September’s content, it’s clear that the St Emlyn’s team has been hard at work bringing you the latest in emergency medicine education and clinical practice. But there’s much more to come.
In the coming months, we’ll be covering exciting topics at upcoming conferences, including the ArchiEM conference in Gateshead and the Slovenia ERC conference. These events promise to bring fresh insights and new perspectives that we’ll be sharing with you through our blog posts and podcasts.
In the meantime, keep doing the incredible work you do in emergency medicine. It’s a challenging field, but it’s also incredibly rewarding, and you’re making a difference every day. Thank you for being part of the St Emlyn’s community, and I look forward to continuing this journey with you.
Stay tuned for more great content, and as always, keep pushing the boundaries of what’s possible in emergency care.

Monday Oct 14, 2019
Ep 148 - CRASH-3
Monday Oct 14, 2019
Monday Oct 14, 2019
The CRASH-3 Trial: Revolutionizing Head Injury Management with Tranexamic Acid
The CRASH-3 trial, a landmark study in the field of emergency medicine, has brought significant attention to the potential role of tranexamic acid (TXA) in managing traumatic brain injury (TBI). As one of the largest randomized controlled trials ever conducted on head injury patients, its findings could reshape clinical practices globally, particularly in the pre-hospital and emergency department settings.
Overview of the CRASH-3 Trial
The CRASH-3 trial was designed to assess the efficacy of TXA in reducing mortality among patients with traumatic brain injury. TXA is an antifibrinolytic agent commonly used to prevent excessive bleeding in various medical scenarios, such as trauma, surgery, and postpartum hemorrhage. The question posed by CRASH-3 was whether TXA could also reduce deaths in patients who had suffered a TBI, a question that had remained unanswered despite the success of the CRASH-2 trial in managing extracranial bleeding.
Patient Population and Inclusion Criteria
The trial focused on adults aged 16 years and older who had sustained a traumatic brain injury. To be included, patients needed to have either a Glasgow Coma Scale (GCS) score of 12 or lower or a positive CT scan indicating intracranial bleeding. Notably, patients with significant extracranial bleeding were excluded from the trial to specifically measure the effect of TXA on TBI outcomes.
A critical aspect of the trial was the timing of TXA administration. Initially, the protocol allowed TXA to be administered within eight hours of injury. However, as data from other studies like the WOMAN trial and CRASH-2 became available, suggesting that the benefits of TXA diminish after three hours, the protocol was adjusted. This change meant that the majority of patients received TXA within three hours of injury, a key factor in the study's final analysis.
Key Findings of the CRASH-3 Trial
The CRASH-3 trial enrolled 12,737 patients across 29 countries, making it one of the most extensive studies of its kind. The primary outcome measured was all-cause mortality at 28 days post-injury. The results showed that overall mortality was slightly lower in the TXA group (18.5%) compared to the placebo group (19.8%), although this difference was not statistically significant.
However, a pre-specified subgroup analysis provided more compelling evidence. When patients with a GCS of 3 and bilateral unreactive pupils (indicating very severe brain injury) were excluded, TXA demonstrated a more significant benefit. In this subgroup, the mortality rate was 12.5% in the TXA group versus 14% in the placebo group, a statistically significant reduction with a relative risk of 0.89. This finding suggests that TXA is particularly beneficial for patients with moderate head injuries (GCS 9-15) who are more likely to survive if bleeding is controlled.
Number Needed to Treat (NNT)
One of the critical metrics for evaluating the effectiveness of a treatment is the number needed to treat (NNT). In the CRASH-3 trial, the NNT was 67, meaning that 67 patients would need to be treated with TXA to save one additional life at 28 days post-injury. For comparison, the NNT for aspirin in acute myocardial infarction is about 42, which is widely regarded as highly effective. An NNT of 67 is therefore quite favorable in the context of emergency medicine, particularly for a condition as serious as traumatic brain injury.
Timing of Administration
The CRASH-3 trial strongly reinforced the importance of administering TXA as early as possible after a head injury. The data indicated a 10% reduction in TXA’s effectiveness for every 20-minute delay in patients with mild to moderate head injury. This underscores the need for TXA to be administered in the pre-hospital setting, ideally by paramedics at the scene or en route to the hospital. Delaying treatment until after arrival at the emergency department or after conducting a CT scan may significantly reduce the drug's benefits.
Implications for Clinical Practice
The results of the CRASH-3 trial suggest that TXA should be considered for all patients with moderate traumatic brain injury, particularly those with a GCS of 9 to 15 and confirmed intracranial bleeding. For patients with severe head injuries (GCS of 8 or less, or with bilateral unreactive pupils), the benefits of TXA are less clear, likely due to the severity of the primary brain injury.
Given the trial’s findings, it is recommended that TXA be integrated into clinical protocols for the management of head injuries. This is especially relevant in pre-hospital care, where early intervention is possible. TXA should be administered as soon as possible after the injury occurs, particularly in cases where a significant delay in getting to the hospital is expected.
Cost-Effectiveness and Accessibility
Another important aspect of TXA is its cost-effectiveness. In the UK, a 1-gram dose of TXA costs approximately £1, making it an affordable treatment option for healthcare systems worldwide. This low cost makes TXA a viable option not only in high-income countries but also in low- and middle-income countries where healthcare resources are often limited. Given its affordability and the potential to save lives, TXA is an attractive option for widespread use in managing traumatic brain injury globally.
Considerations for Special Populations
Although the CRASH-3 trial focused on adults, there is a strong rationale for extending its findings to pediatric patients. The physiology of traumatic brain injury in children is similar to that in adults, and there is no evidence to suggest that TXA would act differently in a younger population. As such, it would be reasonable to use TXA in children with TBI, following the same dosing guidelines adjusted for body weight.
Future Directions: Intramuscular TXA and Beyond
While CRASH-3 has provided valuable insights, research into TXA’s potential uses continues. One area of interest is the development of intramuscular (IM) TXA, which could be particularly useful in pre-hospital settings where intravenous (IV) access is challenging. The possibility of an auto-injector for TXA is also being explored, which could simplify administration and further broaden its use, especially in resource-limited settings.
Conclusion: Implementing CRASH-3 Findings in Practice
The CRASH-3 trial marks a significant advancement in our approach to treating traumatic brain injury. The evidence strongly supports the use of TXA, particularly in patients with moderate head injuries who receive the drug within three hours of injury. TXA is safe, cost-effective, and easy to administer, making it a valuable tool in both pre-hospital and hospital settings.
The implementation of CRASH-3’s findings into clinical practice could save thousands of lives annually, particularly in settings where early intervention is possible. As the emergency medicine community, we must act swiftly to incorporate these findings into our protocols and training, ensuring that TXA is used effectively to improve outcomes for patients with traumatic brain injury worldwide.

Sunday Oct 06, 2019
Ep 147 - August 2019 Round Up
Sunday Oct 06, 2019
Sunday Oct 06, 2019
A Comprehensive Review of St Emlyn’s Blog: August 2019 Highlights
Welcome to St Emlyn’s blog and podcast, where we reflect on the key topics and research from August 2019. In this review, we’ll explore the most impactful discussions and studies, providing valuable insights for emergency medicine professionals. From managing lower GI bleeding and addressing climate change in anaesthesia to examining PTSD in emergency services and the future of diagnostics, this post summarizes essential takeaways that are shaping our field.
Managing Lower GI Bleeding in the Emergency Department
One of the significant topics covered was the management of acute lower gastrointestinal (GI) bleeding, a common but challenging condition in the emergency department (ED). The complexity of managing these cases often lies in determining the correct priority of care, appropriate management strategies, and even the correct speciality for handling these patients.
We reviewed a consensus guideline from the British Society of Gastroenterology and Hepatology, published in Gut, which offers practical recommendations for the diagnosis and management of acute lower GI bleeds. The guideline emphasizes the importance of using stratification tools to distinguish between stable and unstable patients, which can help streamline management in the ED.
For stable patients, the Oakland score is recommended. This scoring system helps identify which patients can be safely managed on an outpatient basis, reducing unnecessary hospital admissions. Conversely, patients with a major bleed should be admitted and scheduled for a colonoscopy at the earliest opportunity. The guideline also highlights the value of CT angiography for hemodynamically unstable patients, a practice increasingly integrated into emergency care.
Transfusion thresholds, set at 70 grams per litre, align with standard practices in other clinical settings, with adjustments for patients with cardiovascular disease. The guideline also recommends having dedicated GI bleed leads within trusts to ensure seamless coordination with emergency services.
Sustainability and Climate Change in Anesthesia
Another crucial discussion from August focused on the environmental impact of healthcare, particularly in anaesthesia. In the UK, healthcare is a significant contributor to climate change, driven by factors like travel, disposable materials, and the use of anaesthetic gases such as nitrous oxide and desflurane.
A key paper by Cliff Shelton and colleagues underscores the need to adopt more sustainable practices in anaesthesia. For example, desflurane is approximately 3,000 times more potent as a greenhouse gas than carbon dioxide. The paper advocates for reducing the use of high-polluting gases and considering greener alternatives where possible.
This shift towards sustainability in healthcare is essential, although challenging, given the nature of medical practice. However, small changes, such as reducing nitrous oxide use in departments where alternatives exist, can collectively make a significant difference. The paper serves as a call to action for healthcare professionals to be more mindful of their environmental impact and to seek sustainable solutions in their practices.
Pre-Hospital Care: Comparing Macintosh and McGrath Laryngoscopes
The debate over the best laryngoscope for pre-hospital rapid sequence intubation (RSI) is ongoing, and in August, we reviewed a study that contributed valuable data to this discussion. Published in Critical Care Medicine, the study compared the Macintosh and McGrath laryngoscopes in pre-hospital settings, involving 514 adult emergency patients.
The study found that both devices were equally effective for pre-hospital RSI. Notably, it also revealed that switching to a different device after a failed intubation attempt was more successful than repeating the attempt with the same device. This finding aligns with the 30-second RSI drills many practitioners use, which advocate for changing the approach after a failed attempt.
These findings have practical implications for both pre-hospital and in-hospital care. In the ED, switching to a video laryngoscope, such as the McGrath, after a failed intubation attempt could improve patient outcomes. As video laryngoscopes become more accessible in emergency departments, integrating them into RSI protocols could be a beneficial strategy.
PTSD in Emergency Services: Rusty Carroll’s Series
Rusty Carroll’s ongoing series on PTSD within the ambulance service continues to be one of the most impactful contributions to the St Emlyn’s blog. The August instalment focused on the aftermath of PTSD, exploring the journey towards understanding what “normal” looks like after such an experience.
Rusty’s candid reflections resonate with many in the emergency services community, highlighting the mental health challenges prevalent in our field. The series has received positive feedback, with many readers finding comfort and validation in Rusty’s experiences.
However, the widespread relatability of this series also underscores a concerning reality: many emergency service professionals are struggling with similar issues. As a community, we need to support one another, promote mental health awareness, and advocate for resources to address the psychological toll of our work. Revisiting Rusty’s previous installments in this series is highly recommended for a deeper understanding of the complex emotions associated with PTSD in emergency services.
The Realities of Packed Red Cell Transfusions
Another fascinating topic from August was the metabolic and biochemical characteristics of packed red cell transfusions, which have significant implications for trauma care in the ED. This discussion was sparked by a conversation on Twitter, leading to critical reflections on the assumptions we hold about blood transfusions.
In trauma care, blood is often regarded as a superior alternative to crystalloids. However, the reality of what we’re transfusing—packed red cells—is quite different from whole blood. A study we reviewed highlighted some surprising statistics about the contents of packed red cells, including a pH of 6.79, a potassium level of 20, and a lactate level of 9.4. These figures reveal that packed red cells are far from the idealized image of whole blood.
The metabolic implications of these characteristics are significant, particularly in the context of massive transfusions. For instance, packed red cells have low levels of 2,3-DPG, which affects their ability to release oxygen to tissues. This raises important questions about how we use blood in trauma resuscitation and whether our current practices are truly optimal.
There’s also an ongoing pre-hospital trial in the UK, known as the RePHILL trial, which is examining the outcomes of patients randomized to receive either blood or no blood in pre-hospital settings. The results of this trial are eagerly anticipated and could challenge the assumption that blood is always better. This could lead to more nuanced transfusion practices in the future.
The Future of Diagnostics: Insights from Rick Body
Finally, we explored the future of diagnostics with insights from Rick Body. His presentation, originally given at the St Emlyn’s Live conference, offers a compelling vision of where diagnostics in the ED is heading. With the rise of machine learning, artificial intelligence (AI), and personalized diagnostics, the landscape of emergency medicine is rapidly evolving.
These technologies are already being integrated into diagnostic processes, but they bring new challenges. The data generated by AI and machine learning can be complex, requiring a shift in how we interpret diagnostic results. We must move away from binary thinking and embrace a more nuanced understanding that includes probabilities, uncertainties, and complexities.
As emergency medicine professionals, we need to prepare for this shift by engaging with these new technologies and incorporating them into our clinical practice. The future of diagnostics is exciting, but it will require ongoing education and adaptation to fully harness its potential.
Conclusion
August 2019 was a month rich with insightful discussions and important research that continue to influence our practice in emergency medicine. From managing lower GI bleeding and the environmental impact of anaesthesia to the complexities of blood transfusions and the future of diagnostics, these topics highlight the diverse challenges and opportunities we face in the ED.
The St Emlyn’s blog and podcast aim to keep you informed and engaged with the latest developments in our field. This review has provided valuable insights that can be applied in your practice, helping you stay ahead in the ever-evolving landscape of emergency medicine. Stay tuned for more updates, and as always, feel free to share your thoughts and experiences with us. Until next time, take care and continue to push the boundaries of what’s possible in emergency medicine.

Saturday Oct 05, 2019
Ep 146 - European Resus Council meeting Slovenia 2019
Saturday Oct 05, 2019
Saturday Oct 05, 2019
A vox pop round up of the best of the ERC19 conference in Slovenia.

Friday Sep 27, 2019
Ep 145 - The UK Resuscitationist with Dan Horner at #stemlynsLIVE
Friday Sep 27, 2019
Friday Sep 27, 2019
Our latest podcast from the #stemlynsLIVE conference last year. Dan Horner talks on the concept and potential role of the UK Resuscitationist.

Tuesday Sep 10, 2019
Ep 144 - July 2019 Round Up
Tuesday Sep 10, 2019
Tuesday Sep 10, 2019
St Emlyn’s July 2019: Key Highlights
Welcome back to St Emlyn’s, where we continue to share the latest insights, discussions, and advancements in emergency medicine. July 2019 was particularly rich in content, covering a wide range of topics from practical clinical advice to deeper reflections on the ethics and philosophy of emergency medicine. Here, we summarize the key points from the month’s posts, optimized for clarity and relevance.
Upcoming Events: Resuscitology Course and MSc in Emergency Medicine
Before diving into the content highlights, there are two important announcements:
Resuscitology Course – December 2019
On December 14th, 2019, the Resuscitology course will be held in Manchester. This course, led by Cliff Reid, offers an in-depth exploration of why certain resuscitation techniques work and how they can be improved in high-stakes scenarios. This is a must-attend for anyone involved in emergency or critical care. Registration details are available on our blog.
MSc in Emergency Medicine – 2019-2020 Cohort
Recruitment is now open for the 2019-2020 cohort of the MSc in Emergency Medicine. This three-year online program, available to both doctors and nurses, offers an advanced curriculum in emergency medicine. Alumni like Janus Bae, Alan Grace, and Natalie May have found it immensely beneficial. By 2020, we hope to extend the program to paramedics as well, broadening its reach and impact.
July 2019 Blog Highlights
This month’s content ranged from clinical insights and research updates to philosophical discussions about the practice of emergency medicine.
Disaster Medicine in Pakistan: Lessons Learned
Zaf Kasim, now practicing in the United States, and Rashid Akhil from Pakistan collaborated on a blog post discussing the management of natural disasters, terrorist attacks, and major incidents in Pakistan. Zaf, who trained with us in Verchester, has become an authority in endovascular resuscitation, REBOA, and ECMO.
This post sheds light on the expertise developed by medical professionals in Pakistan, particularly in response to large-scale disasters like the 2005 Kashmir earthquake. It’s a crucial read for anyone interested in global health or disaster medicine, as it demonstrates how effective disaster response systems can be developed even in resource-limited settings.
Managing Major GI Hemorrhage: Practical Insights
Chris Gray revisited a talk he gave at the St Emlyn’s Live Conference, focusing on the challenges of managing major gastrointestinal (GI) hemorrhage. Patients presenting with significant upper or lower GI bleeds pose unique challenges, particularly regarding airway management.
Chris offers practical advice, emphasizing the importance of resuscitating before intubation and considering video laryngoscopy in difficult cases. The post also highlights the SALAD (Suction Assisted Laryngoscopy and Airway Decontamination) technique, which is particularly useful in managing patients with large amounts of gastric contents.
Additionally, Chris touches on the use of PPIs, tranexamic acid (TXA), and terlipressin, although he advises caution until more evidence is available. The ongoing HALT-IT trial in the UK, investigating TXA in GI bleeds, is something to watch closely.
Listeriosis: A Rare but Serious Infection
Listeriosis, though uncommon, can have severe consequences, particularly for vulnerable populations like the elderly, pregnant women, newborns, and the immunocompromised. This blog post was prompted by a recent outbreak in the UK linked to contaminated hospital food.
The post emphasizes the importance of considering listeriosis in differential diagnoses, particularly for patients presenting with unexplained gastrointestinal symptoms. Blood cultures are essential for diagnosis, making it important to include them in the workup for high-risk patients. Early diagnosis is key to improving outcomes in these cases.
The Procedure Paradox: Ethical Reflections in Emergency Medicine
“The Great Day Paradox” delves into the ethical and emotional challenges of emergency medicine. Inspired by a talk at the Don’t Forget the Bubbles conference, this post explores the contrast between the excitement clinicians feel during life-saving procedures and the often devastating impact these events have on patients.
The post encourages clinicians to reflect on their motivations and maintain a patient-centered approach. Drawing on the teachings of John Hinds, it emphasizes that every procedure should be justified by both clinical need and appropriateness for the patient. This blog is a reminder of the importance of balancing clinical enthusiasm with compassion and ethical care.
Inferior Vena Cava Filters in Major Trauma: An Evidence-Based Review
Rich Carden reviewed the use of inferior vena cava (IVC) filters in major trauma patients, a topic that has been debated for years. IVC filters are intended to prevent pulmonary embolism (PE) in high-risk patients, such as those with significant lower limb or pelvic fractures.
Rich discusses a recent randomized controlled trial published in the New England Journal of Medicine, which found that early prophylactic use of IVC filters did not reduce the incidence of symptomatic pulmonary embolism or death at 90 days. This finding suggests that IVC filters should not be used routinely in major trauma patients, though there may be specific cases where they are warranted.
Psychological Performance in the Resus Room: Insights from Texas
Ashley Leibig’s presentation at St Emlyn’s Live focused on psychological performance in the resus room, drawing on her experience with StarFlight in Texas. Her blog post explores key concepts such as human factors, crew resource management, and self-awareness in high-pressure situations.
Ashley’s practical advice on managing oneself, the team, and the environment in emergency medicine is invaluable. This post is essential reading for anyone looking to improve their performance under pressure, whether in emergency medicine or other high-stress fields.
The Resuscitative Care Unit: A New Model for Emergency Departments
The concept of the resuscitative care unit (RCU) or ED-based critical care units was the focus of our final post of the month. Inspired by a paper published in the Emergency Medicine Journal (EMJ), this blog discusses the idea of creating RCUs to serve as a bridge between the emergency department and intensive care.
RCUs are proposed as a solution for managing critically ill patients who require short-term intensive care but may not need full ICU admission. The post also references a JAMA study showing that ED-based ICUs can improve survival rates for critically ill patients. As emergency departments continue to evolve, integrating critical care capabilities is becoming increasingly important.
Conclusion
July 2019 was a month filled with rich, varied content at St Emlyn’s, offering practical advice, research updates, and philosophical reflections on emergency medicine. Whether you’re interested in disaster management, GI haemorrhage, or the ethical challenges of our profession, this month’s highlights provide valuable insights.
We encourage you to engage with our content, share your thoughts, and continue learning. Don’t forget to check out our upcoming events, including the Resuscitology course and the MSc in Emergency Medicine. If you find our content valuable, please consider supporting us through a small donation to help keep St Emlyn’s free and accessible to all.
Thank you for being part of the St Emlyn’s community. We look forward to bringing you more valuable content in the coming months.

Saturday Aug 31, 2019
Ep 143 - The Future of Diagnostics with Rick Body
Saturday Aug 31, 2019
Saturday Aug 31, 2019
Prof. Rick Body is an internationally recognised expert in diagnostic testing. In this podcast he takes us through diagnostics today and also the near future which may change almost everything.
You can read more and see the slides/video at http://www.stemlynsblog.com

Tuesday Jul 23, 2019
Ep 142 - Psychological performance in the Resus Room with Ashley Liebig
Tuesday Jul 23, 2019
Tuesday Jul 23, 2019
This talk focuses on how we can optimise our psychological performance in critical care situations, the type of situations that Simon describes as Time Critical, Information light. The Audio is available below, or watch the full presentation above.
Don't forget to watch the video on the St Emlyn's site http://www.stemlynsblog.org
vb
S
